 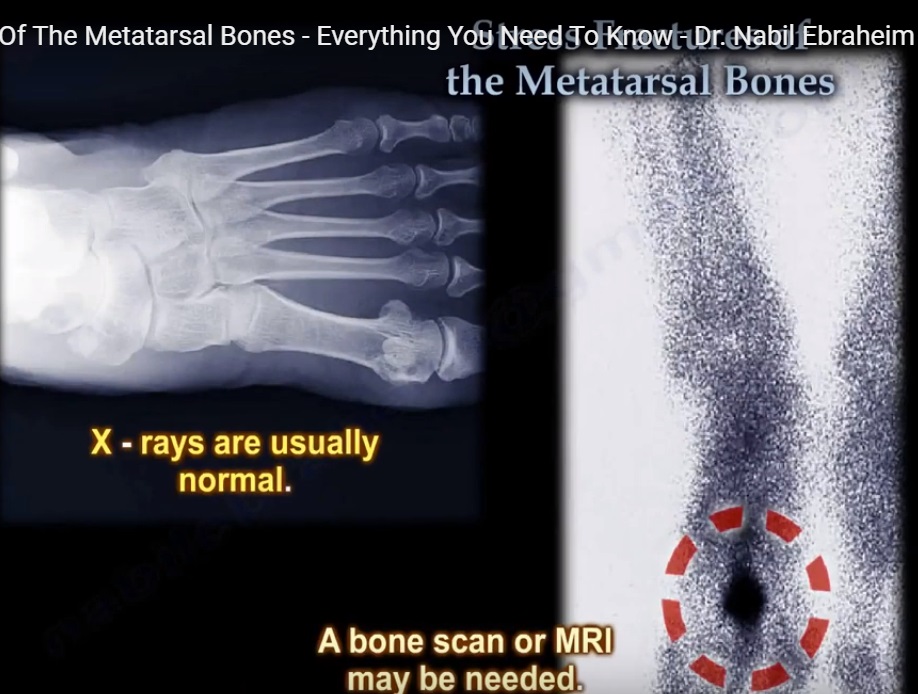
The preferred method of revision treatment is intercalary autogenous bone grafting and dorsal plating. Several techniques have been described to revise these nonunions. Highly comminuted or segmental fractures of the metatarsal diaphysis can result in painful nonunion. The treating physician may be tempted to address the symptomatic metatarsal however, correcting the malunited metatarsal is more prudent. When there is a dorsiflexory sagittal plane malunion, the patient will present with symptomatic metatarsalgia juxtaposition to the malunited metatarsal. Much like metatarsal head malunions, a sagittal plane malunion of the shaft is corrected with realignment osteotomies. This will prevent sagittal plane malposition of the metatarsal. The external fixation bars should be oriented parallel to the long axis of the metatarsal. The surgeon should pay close attention to the metatarsal declination angle when using external fixation. This technique is most useful in highly comminuted or open fractures. Another option for stabilizing these fractures is external fixation. This provides stabilization of the fracture without disrupting the biology around the fracture. Bridge plating allows the surgeon to “bridge or span” the comminuted segment while concurrently receiving osseous stability from the bone proximal and distal to the area of comminution. Bridge plating works well for comminuted metatarsal shaft fractures. Deviation from this technique can lead to healing complications including nonunion and malunion. Because of this, additional dorsal plating is recommended for neutralization. The perpendicular placement of this screw is challenging due to inference of the adjacent metatarsals. Spiral fractures should be stabilized with interfragmentary fixation. A vertical oriented fracture can be treated in with a 0.062 in. When the fracture is displaced and surgical treatment is being considered, the pattern of the fracture helps determine the most appropriate fixation. Certain fracture patterns of the metatarsal shafts are more appropriately treated with surgical stabilization. 10.2).įractures of the central metatarsal diaphysis are often treated nonsurgically as well. A dorsal wedge is removed from the metatarsal head, and the viable plantar cartilage is rotated dorsally (Fig. These osteotomies use the viable and uninjured plantar cartilage to interface with the base of the proximal phalanx. 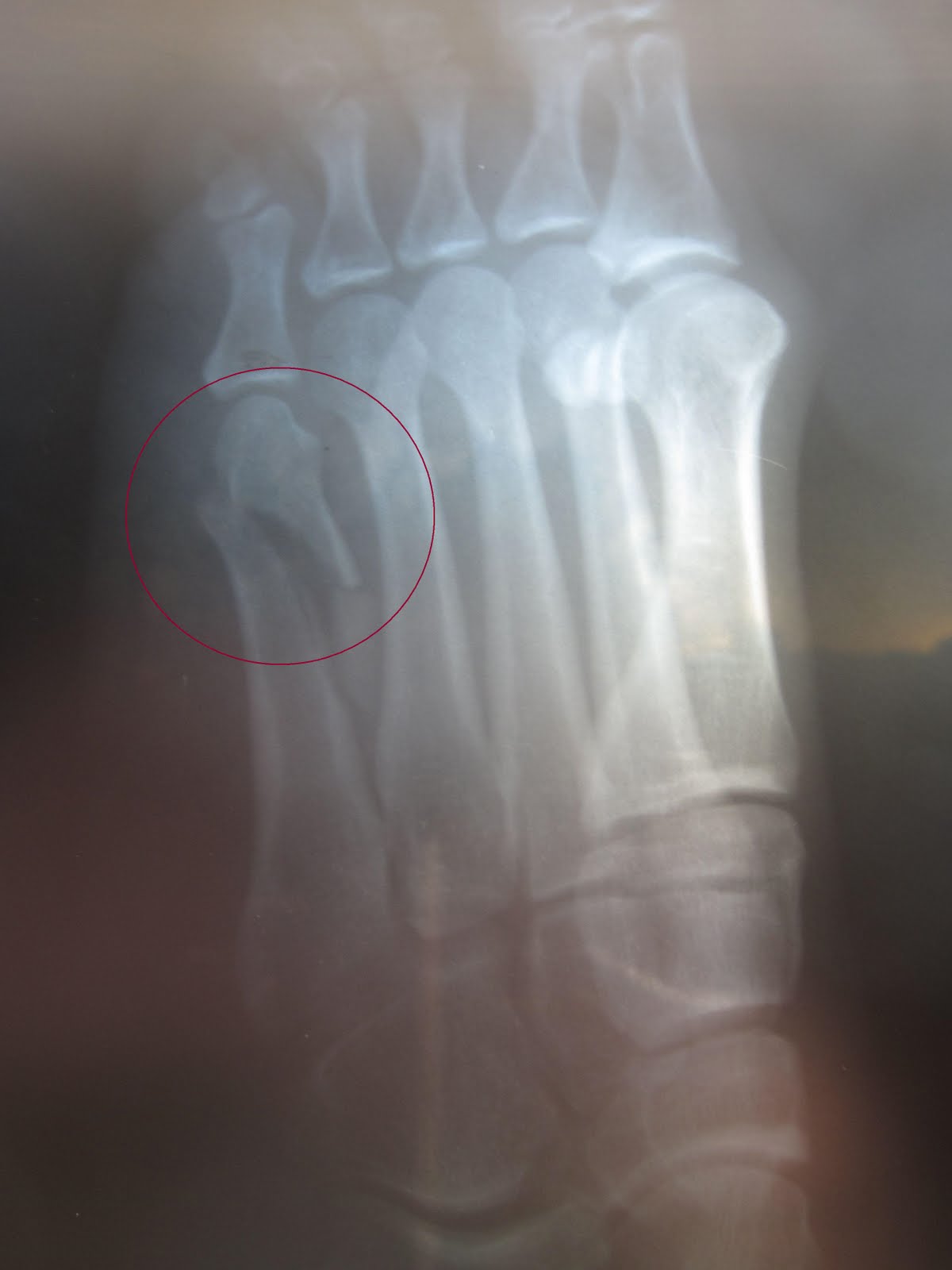
Rotational dorsal wedge osteotomies have shown to be an excellent option. If the articular insult is large, excision is not recommended and more advance reconstructive techniques should be considered. If the fragment is small, simple excision is sufficient treatment. The treatment depends on the size of the fragment. These treatments include debridement, excision, synovectomy, and dorsal closing-wedge osteotomy. However, several authors have described a variety of applicable treatments for osteochondral defects of the metatarsal head. The majority of the literature pertains to reconstruction of avascular necrosis. 
Osteochondral injuries are often caused by axial load, and the cartilage surface sustains a shear-type injury. Zone 2 injuries may involve acute or stress fractures, but all are at higher risk of nonunion from possible disruption of the more tenuous blood. Spiral fractures of the distal shaft of the fifth metatarsal are common injuries and can usually be treated nonoperatively for these high performance athletes without long-term functional sequelae.Complication of these injuries can result in osteochondral defects, avascular necrosis, or more commonly sagittal plane malunion. These fractures extend transversely towards the intermetatarsal joint (between the bases of fourth and fifth metatarsal) and/or into the proximal diaphysis just distal to the intermetatarsal joint. All patients returned to professional performance without limitation and no patient reported pain with performance at followup. There was one delayed union (7 months) and one refracture (2 months) that subsequently healed. The average time to pain free walking was 6.1 weeks (range, 0 to 16) return to barre exercises, 11.6 weeks (range, 4 to 48) and return to performance, 19 weeks (range, 6 to 52). Patients with marked displacement of the fracture underwent internal fixation early in the study period but more recent treatment emphasized nonoperative means, even for displaced fractures. Treatment consisted of open reduction and internal fixation for 2 patients, closed reduction and percutaneus fixation for 2 patients, short leg weightbearing cast for 7 patients, and an elastic wrap and treatment of symptoms for 24 patients. The usual fracture pattern is a spiral, oblique fracture starting distal-lateral and running proximal-medial. We retrospectively reviewed the office records of the senior author-which include two national ballet companies-and identified 35 dancers who sustained distal shaft fractures of the fifth metatarsal. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
